Condition
Neck Pain After a Car Accident
Cervical spine injuries from car accidents range from muscle strain to disc herniation and facet joint damage. Accurate diagnosis is essential to differentiate mechanical pain from neurological involvement and to document the full extent of your injury.
Understanding the Injury
What Causes Neck Pain After an Accident?
The cervical spine is a complex structure comprising seven vertebrae, intervertebral discs, paired facet joints, multiple ligaments, and layers of muscle. During a car accident, the forces transmitted through the neck can injure any combination of these structures, producing neck pain that ranges from mild muscular discomfort to severe, debilitating pain with neurological involvement.
The specific pattern of injury depends on collision direction, seat position, head restraint height, and whether the impact was anticipated. Rear-end collisions tend to produce extension-flexion whiplash injuries. Side impacts can cause lateral flexion injuries. Frontal collisions may cause pure flexion injuries or compression fractures. Each mechanism damages different structures and requires different evaluation strategies.
Why Diagnosis Matters
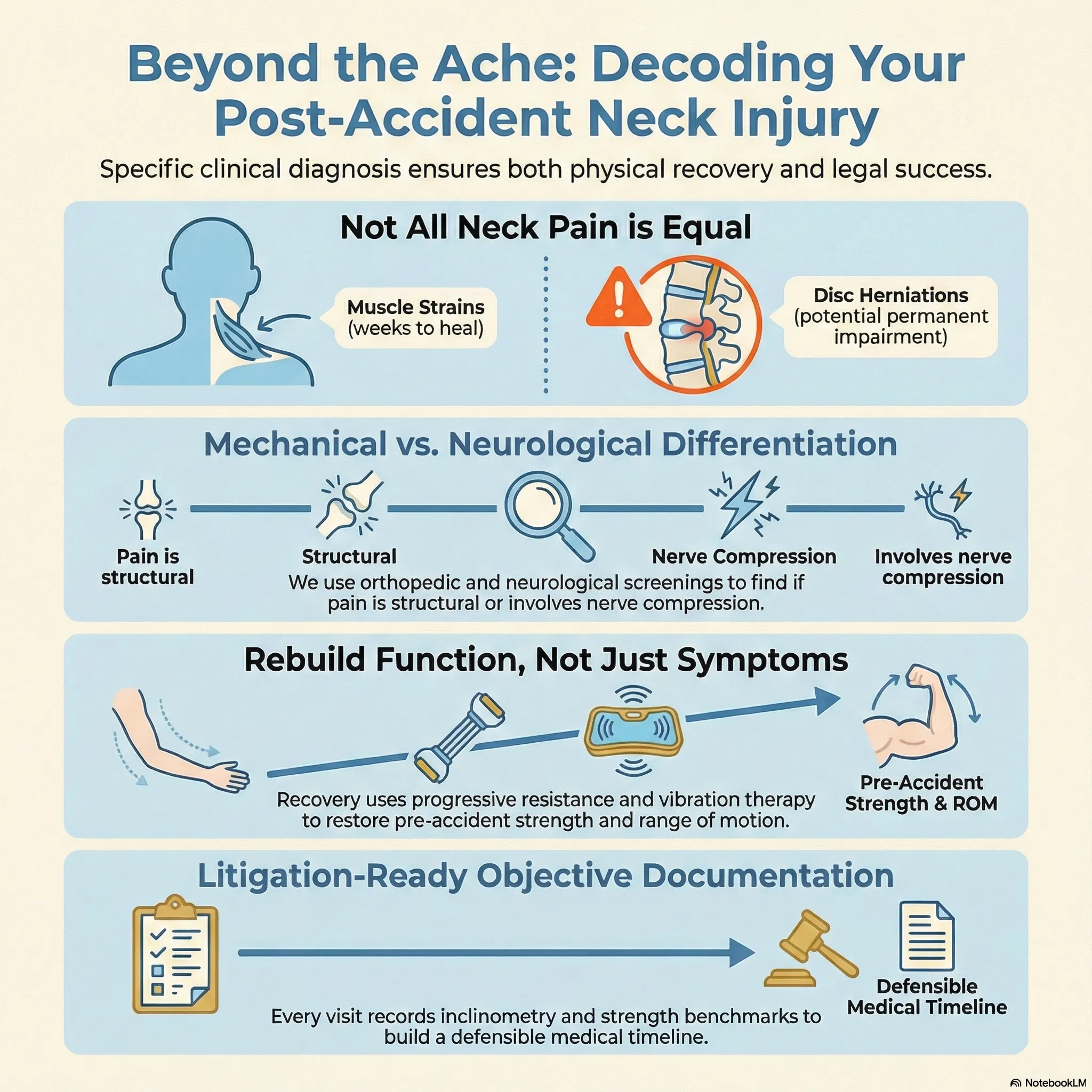
Not all neck pain is the same. Cervical muscle strain, disc herniation, facet joint capsule injury, and nerve root compression all produce neck pain, but they require different treatment approaches and carry very different implications for your case. A cervical strain may resolve in weeks, while a disc herniation with radiculopathy may represent a permanent impairment.
Differentiating between mechanical neck pain and neurological involvement requires a thorough orthopedic and neurological examination, which is exactly what we provide at every initial evaluation.
Cervical Strain
Muscle and tendon injuries from overstretching during the collision. Produces pain, stiffness, muscle spasm, and cervicogenic headaches. Can involve deep cervical flexors, extensors, and lateral stabilizers.
Disc Herniation
The intervertebral disc bulges or ruptures under compressive and shearing forces. Can compress adjacent nerve roots, producing radiating arm pain, numbness, tingling, and weakness.
Facet Joint Injury
The paired facet joints that guide cervical motion can sustain capsular tears and cartilage damage. Produces localized neck pain that worsens with extension and rotation.
Radiculopathy
Nerve root compression from disc herniation or foraminal narrowing. Causes radiating pain, numbness, or weakness into the shoulder, arm, or hand along specific dermatomal patterns.
Diagnosis
How We Diagnose Neck Pain
A comprehensive cervical spine evaluation that identifies every injured structure and differentiates mechanical pain from neurological involvement.
Orthopedic Examination
Systematic evaluation of the cervical spine's bony, discal, and soft tissue structures.
- Cervical range of motion with inclinometry
- Spurling's test for radiculopathy
- Cervical compression and distraction
- Facet joint provocation testing
- Muscle palpation and trigger point mapping
- Shoulder depression test
Neurological Screening
Full upper extremity neurological assessment to identify nerve root involvement.
- Upper limb dermatome testing (C4-T1)
- Myotome strength grading
- Deep tendon reflexes (biceps, triceps, brachioradialis)
- Sensory discrimination testing
- Upper motor neuron screening
- Cranial nerve assessment for TBI screening
Imaging Coordination
Advanced imaging referral when clinical findings indicate structural pathology.
- MRI for disc, ligament, and cord evaluation
- Flexion-extension radiographs for instability
- Digital motion X-ray when indicated
- CT referral for bony pathology
- Clinical-imaging correlation report
- Pre- and post-imaging comparison
Treatment
How We Treat Neck Pain
Progressive, movement-based rehabilitation that addresses the specific structures involved and rebuilds functional capacity from the ground up.
Progressive Resistance Training
Restores cervical strength and endurance lost after injury. We target the deep cervical flexors, extensors, and lateral stabilizers with graded resistance exercises that rebuild stability and movement confidence along functional lines of force.
Cervical Strengthening ProtocolVibration Therapy
Reactivates the cervical proprioceptive system disrupted by injury. Whole-body vibration challenges the deep stabilizers of the cervical spine, retrains balance, and restores the neuromuscular coordination essential for head-on-neck control.
Proprioceptive RetrainingFocused Shockwave Therapy
Targets chronic myofascial pain, muscle spasm, and fibrotic tissue that can develop after cervical injury through targeted soft tissue therapy. Acoustic energy breaks up adhesions in the cervical musculature and stimulates cellular repair in damaged soft tissues.
Myofascial ReleaseChiropractic Adjustments
Precise spinal manipulation to restore segmental mobility in fixated cervical joints. Addresses the biomechanical restrictions caused by injury, reduces facet joint dysfunction, and creates the mobility foundation for effective rehabilitation.
Segmental Mobility RestorationMeasurable Recovery at Every Visit
Each treatment session documents objective data: cervical range of motion measurements, strength benchmarks, pain ratings, and functional capacity assessments. This builds the progressive recovery timeline that shows improvement, justifies treatment necessity, and supports your personal injury case from day one through maximum medical improvement.
Defensible Medical RecordsWhy adjust.clinic
What Makes Us Different
We don't treat all neck pain the same way. We diagnose the specific injury, treat the specific structures, and document everything with the precision that personal injury cases require.
-
📋
QME Designation
Dr. Lloyd's Qualified Medical Evaluator certification means his diagnoses, treatment plans, and impairment ratings carry the authority of an independent medical examiner.
-
🔬
Mechanical vs. Neurological Differentiation
We perform the orthopedic and neurological testing needed to determine whether your neck pain involves nerve compression, disc injury, or is primarily muscular. This distinction shapes treatment and case value.
-
🏃
Function Over Symptom Management
Our goal is restoring the range of motion, strength, and endurance your neck had before the accident. Every treatment is aimed at rebuilding function, not just reducing pain scores.
-
⚖️
Litigation-Ready Reports
Every neck pain case generates detailed documentation: mechanism of injury, clinical findings, diagnosis, treatment records, and outcome data formatted for personal injury attorneys, demand packages, and courtrooms.

Common Questions
Frequently Asked Questions About Neck Pain After a Car Accident
What's the difference between cervicalgia and radiculopathy?
Cervicalgia is localized neck pain — the muscles, joints, and ligaments of the cervical spine are injured but nerves are not compressed. Radiculopathy occurs when a damaged disc or swollen tissue presses on a nerve root, causing pain, numbness, or weakness that radiates into the shoulder, arm, or hand. The distinction matters because radiculopathy typically indicates a more severe injury with different treatment and documentation requirements.
Why does my neck pain get worse days after the accident?
Delayed onset is extremely common with car accident neck injuries. Adrenaline and inflammation masking can suppress symptoms for 24–72 hours. As the body's acute stress response fades and soft tissue swelling increases, pain and stiffness intensify. This is why early evaluation is critical — even if you feel fine at the scene.
When should I get an MRI for neck pain after a car accident?
An MRI is indicated when symptoms include radiating arm pain, numbness or tingling in the hands, progressive weakness, or neck pain that doesn't improve with 4–6 weeks of conservative care. Dr. Lloyd orders MRI when clinical findings suggest disc herniation, ligament damage, or spinal cord involvement that X-rays cannot detect.
How long does neck pain treatment take after a car accident?
Mild cervical strains typically resolve in 6–8 weeks. Moderate injuries with joint dysfunction or muscle guarding may take 8–12 weeks. Disc injuries, facet joint damage, or radiculopathy often require 3–6 months to reach maximum medical improvement. Treatment duration is documented throughout for your personal injury case.
Do I need to pay out of pocket for neck pain treatment after my accident?
No. Adjust Clinic provides lien-based care for personal injury patients, meaning you pay nothing until your case settles. If you have MedPay coverage on your auto policy, we can bill that directly for immediate treatment coverage with zero out-of-pocket cost to you.
Neck pain after your accident?
Get a thorough cervical spine evaluation that identifies every injury and documents it for your case. Same-week appointments available.
Have MedPay on your auto insurance? Learn how to use it here.
Learn more about our car accident chiropractic care in Petaluma.
Related Conditions
Other Conditions We Treat
Neck injuries frequently occur alongside other collision injuries. Explore the conditions we specialize in.